Where Dental Care Isn’t Reaching, They Go
Mobile dental teams in U.S. rural and low-income areas provide essential care to underserved populations lacking access to traditional services.
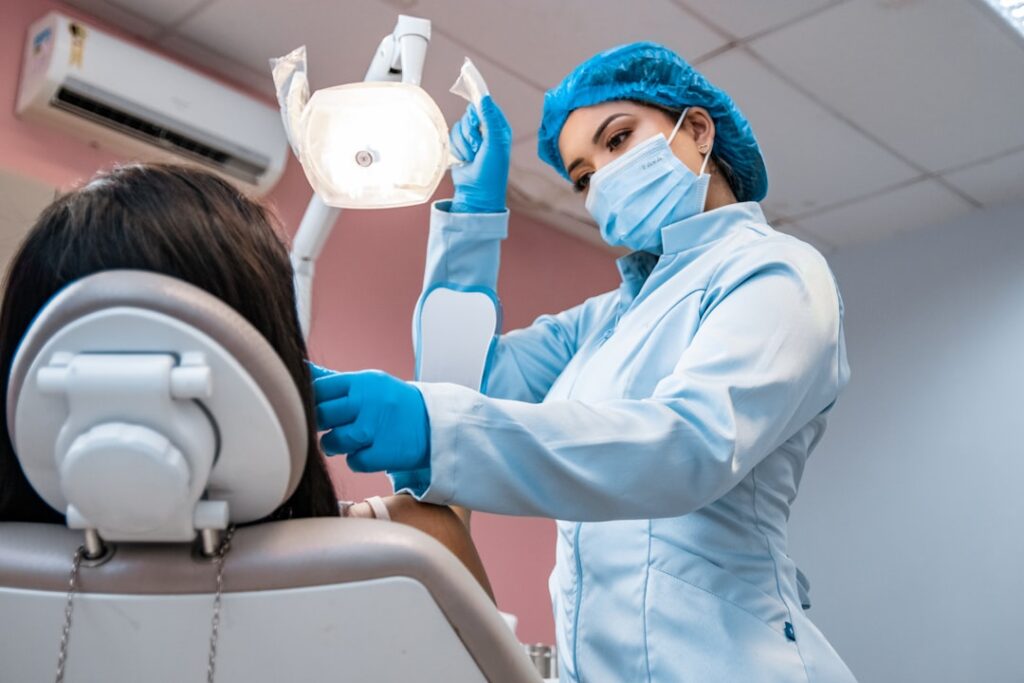
Image: GlobalBeat / 2026
Dental care access: Mobile clinics erase 120-mile gaps for Tennessee rural patients
Sarah Mills | GlobalBeat
A fleet of three retrofitted vans now covers 120-mile dead zones across West Tennessee where no dentist practices, delivering cleanings, fillings and extractions to 3,400 patients in its first 18 months.
The program run by the University of Tennessee Health Science Center parks in school lots, church driveways and feed-store parking areas on a fixed two-week rotation, filling cavities the same day because many clients have no transport back.
Rural counties outside Memphis lost 38% of their dental providers between 2010 and 2022, according to state licensing records, leaving 1 in 4 adults with untreated decay that emergency rooms can only quiet with antibiotics. The vans carry portable X-ray units, steri-center and a generator that hums louder than the drill, letting two faculty dentists and six students treat 18 patients per stop instead of referring them hours away.
“People line up at 6 a.m. for a 9 o’clock slot,” said Dr. James Francomano, the project director, who logs 2,100 miles a month. “One farmer pulled his own tooth with pliers because the ache kept him from harvesting soybeans.”
State data shows $17.4 million spent in 2023 on dental-related ER visits that offered no actual dentistry, a bill the mobile unit slashes to roughly $180 per encounter. Medicaid covers 72% of the van patients, yet Tennessee reimburses only 70% of urban rates, so the college subsidizes fuel and student stipends with a $1.2 million federal grant awarded in 2023.
The scarcity is starkest in eight counties bordering the Mississippi River. Lake County has zero licensed dentists for 7,600 residents; Lauderdale lists two, both over 60. Weak Medicaid fees, aging populations and hospital closures form what Francomano calls “a perfect storm of silence” — nobody drills, so pain becomes normal.
Students swap the polished clinic floor for cracked asphalt and wind that whips cottonwood through open doors. They learn to chart decay by head-lamp after sunset when the generator fuel runs low. “You feel the pressure — this may be someone’s only shot for years,” said fourth-year student Dana Robles after extracting an infected molar from a 34-year-old trucker outside Ripley.
Mobile programs exist in 42 states, but Tennessee’s twist pairs each patient with a telehealth enrollment scribe who schedules a follow-up before the van leaves. One clipboard swipe secures transportation vouchers and flags diabetics for primary-care slots back in Memphis, tightening a gap that usually drops people back into limbo.
James Harris, 58, wore silver duct tape on his glasses to hold the arm when he arrived at the Dyersburg fairground site. Abscesses had kept him awake since New Year’s. Thirty minutes later he stepped off with two fillings, a referral for hypertension meds and a next appointment already in his flip phone. “I thought I’d have to pull them out myself next,” he said, tongue probing the new composite.
Local mayors lobby for the schedule like concert promoters. Haywood County’s Allan Sterling reserved the central courthouse square because foot traffic is heavier than at the health department on the hill. “Word spreads when the white vans roll in,” Sterling said. “Main Street fills up, and the diner brings out sandwich boards.”
Legislators took notice. A bipartisan bill moving through Nashville would add $450,000 yearly to clone the model in Appalachian East Tennessee, where driving times to the nearest chair average 94 minutes. The funding amendment passed the House health subcommittee 15-2 last week, attaching dental vans to the state’s existing mobile mental-health fleet.
Skeptics warn the vans may skim the healthiest patients, leaving complex oral surgeries untouched. “Mobile units do hero work, but they can’t place implants or treat advanced gum disease,” said Dr. Kathy Wood, president of the Tennessee Dental Association, which instead lobbies for higher Medicaid fees statewide. She noted that three mobile programs closed in Kentucky after grants expired, stranding patients again.
Francomano keeps a running wait-list that tops 600 names. He rotates extraction days with preventive clinics because demand for both outstrips chair time. “Our goal isn’t to replace an entire dental system,” he argued. “It’s to stop infection, pain and tooth loss until the system rebuilds.”
Background
Rural dental shortages widened after the 2007 recession, when 1,117 private practices nationwide shuttered and newly minted dentists clustered in cities offering higher incomes and shared-tech suites. Tennessee compounded the gap by refusing Medicaid expansion for working adults until 2021, leaving large numbers without coverage just as older clinicians retired.
Federal workforce data counts 6,350 Dental Health Professional Shortage Areas across the United States, covering 67 million residents. Mobile clinics originated in the 1970s but rebounded after 2010 when portable suction and digital X-ray units shrank to carry-on size. Studies by the American Dental Association show each dollar spent on preventive van visits saves $11 in later ER fees.
What’s Next
UTHSC will deploy a fourth van in September if the state budget amendment clears the Senate, targeting three additional counties near the Kentucky border. Administrators anticipate serving 6,000 patients annually by 2027, pending renewal of the federal grant that expires in October 2025.
Technology & Science Editor
Sarah Mills is GlobalBeat’s technology and science editor, covering artificial intelligence, cybersecurity, public health, and climate research. Before joining GlobalBeat, she reported for technology desks across Europe and North America. She holds a degree in Computer Science and Journalism.